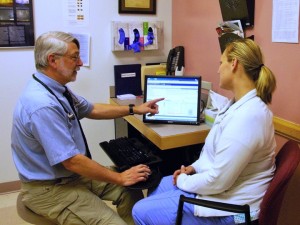
SPM board member Peter Elias MD viewing medical record with patient
The other night I participated in a very useful Google+ hangout with SPM members Adrian Gropper and Michael Mascia, and Michael Chen [of NOSH, explained below]. The discussion focused on a subject I think is incredibly important: the patient-centered health record.
Really: patient-centered. Like, built around the patient – not a provider system built with supposed “patient-centered” thinking.
This topic is hard to discuss without drowning in technical terms and acronyms. I consider myself fairly tech-savvy and still struggle. So I’m going to describe the idea first without tech terms or acronyms, and then with some of the key jargon added, so more technical readers can see what we’re specifically proposing.
The 55 minute YouTube replay of the hangout is embedded at the end of this post. I think it is worth watching. Before watching it, consider reviewing the following basic information to help set the stage.
Our situation today
The current EHR model is that each office or institution owns and manages an electronic record that contains information about the patients in that system. Despite the obvious need and lots of talk, there has been little actual progress towards making these separate and mostly proprietary systems ‘interoperable’ and therefore able to share information. The result is that
- Clinicians routinely work with incomplete or outdated information.
- Patients are locked into their home system.
- It is extremely hard for patients to access their own information in any meaningful or useful way.
- Care is less safe and less reliable, patients are prevented from actively managing their care, and clinicians are frustrated.
This is a problem. Lots of problems, actually.
Our proposed model, without acronyms
The model discussed in this video takes a different approach, one that appeals to me for both philosophical and technical reasons. In this model:
- The basic unit is a one-patient record unique to the individual patient.
- It is ‘open source’ meaning that the code is public, maximizing the ability to improve or modify it and create added pieces for new functions.
- This basic unit and its information are owned and controlled by the patient.
- This is where all the health and medical information about an individual patient is stored.
- It contains the most current, complete and up-to-date information.
- The patient has full access to their individual record.
- This patient-centered health record has a component that allows the patient to control access by others, essentially inviting their clinicians (or others) to see and use the information.
- This is not unlike how users of Quicken and Mint.com own their data, and grant access to accountants etc.
- Clinicians can access the system through their own software using one of two mechanisms:
- Using a straightforward process which gives them access to multiple separate patient records, and they work in the actual patient record. Or,
- Using their proprietary clinician or institution owned system, which is linked to and synchronized with the patient’s individual record (through a software interface, described below).
- In both cases, the ‘official’ version of the information is the patient-centered / patient-owned record, fully accessible to the patient.
- This is important because it’s not uncommon for two different EMRs to disagree about a patient’s medical facts. In such situations, computer science and quality control demand that there be agreement about which record is considered “the bible.”
- There are standardized connections between the clinician-based systems and the multiple patient-based records.
With technical details:
That was English. Now a version of the same information with some jargon:
- The patient has a record (EHR) to store his or her health information
- Ideally it is ‘open source’ software such as NOSH (New Open Source Health Charting System) by Michael Chen. Read more about this at https://NoshEMR.wordpress.com/.
- It is owned and controlled by the patient.
- It is where all the health information about an individual patient is stored.
- It functions as the ‘Source of Truth.’ [“The bible” as described above]
- The patient has full access.
- The patient-centered record (such as NOSH) has a component that allows the patient to control who can see, change or use the information.
- This is sometimes called UMA (for User Managed Access).
- It has other names such as HIE of One (health information exchange of one).
- This is what allows the patient to manage who has access.
- Clinicians access the system (the patients’ data) through their own software using one of two mechanisms:
- They use a parallel open-source software system that has a list of the patients using individual patient records they have been authenticated to use. Or…
- They use (work in) their institution’s proprietary system which is linked to and synchronized with the official patient-owned record.
- In both cases, the patient’s record is the Source of Truth and fully accessible to the patient.
- There are interfaces that make connections work.
- FHIR (pronounced fire) is the one talked about here.
- Other ‘application program interfaces’ (APIs) can be developed or used, especially if the system is open source.
Key design principles
There are several important considerations in a system like this:
- Open source software improves security, adaptability, flexibility.
- This is based on the assumption that patients should have full control over their health information according to their own needs, not just be given limited access by clinicians or their systems.
- If patients have full control over access to their health information, it goes without saying that they can access their own health information without either delay or barriers.
- It can be adopted incrementally rather than requiring the entire US healthcare system to turn a switch all at once. (Patients can start using it whenever they want, and providers can plug into it whenever they want.)
Our call to action:
Patients and clinicians can help us move from where we are now to a patient-centered health record system by:
- Understanding the concept.
- Being at least somewhat familiar with the terminology.
- MAKING NOISE about wanting a system like this in their local setting.
What do you think?
If you’re interested, here’s the 55 minute YouTube replay of the Hangout where we discussed this.
Members of our Society for Participatory Medicine [join here] can participate in discussions on our member listserv. Like many forums, ours is sometimes noisy and scattered (ahem, wide-ranging?), but they’re also home to some great threads. The post above is a message posted Saturday by SPM board member-at-large Peter Elias, a recently-retired primary physician in Maine. It’s already been cross-posted by THCB, The Health Care Blog.






This is an excellent summary in English and again with jargon.
Thanks to all who organized the Hangout and put this together.
This definitely makes the case for being snowed in. Seriously, this is a very cogent and clear statement not only of a technological solution, but of the fundamental dynamics and principles necessary to come to a solution. One patient, one record, patient controlled helps reconcile (if not completely settling) issues of ownership, timely access, accuracy, privacy, and identity/patient identification.
For those who don’t know, @DCPatient (her Twitter name) is Donna Cryer (DC) who lives in DC. Her health history is prodigious, so she knows whereof she speaks.
Meanwhile, just to illustrate how “Homer Simpson” / “Doh!” this is, last week Medscape ran another article The Case for a Patient-Centered EHR: My Dad … and it’s behind their paywall.
Excerpt: “we need a shift toward thinking about the medical record as centered around the patient, not the doctor. For the most part, we have designed medical records that mimic paper charts, which by their nature are intended for local consumption rather than a contribution to a larger whole.“
@e-Patient Dave: I am not sure, but I think one can register for a free account on Medscape.
Good argument for a shift in the Health IT market.
Suggest you need to look at the openEHR architecture, methodology and tooling.
A few more related links of interest.
frectal.com/2014/06/30/21stc-healthcare-open-platform/
rippleosi.org
Keep up the open platform push
regards
Tony
You’re definitely heading in the right direction. There needs to be a major shift in the way our provider-based EMRs are architected, and putting the individual patients’ records at the center is the right approach. What I think will be needed though is a mechanism to ensure the integrity of professionally sourced information in the records. A patient’s record needs to tell a complete and accurate story, even if the patient doesn’t appreciate what it is stating. The patient needs a process to dispute, but should not be able to erase or alter professionally sourced information in the record.
8-9 years ago, Google tried to establish a patient-centered EMR. It was shut down 3 years ago. There were many reasons for its demise. But the two primary reasons were:
1. It was costing Google too much to build relationships with providers, including medical labs.
2. Active and healthy consumers were not incentivized to participate.
Microsoft’s HealthVault is currently active. They have built relationships with hundreds of providers. They also have an emphasis on tracking fitness/diet issues. They even offer an electronic link to fitbit so that when you link your Fitbit account with a HealthVault record, Fitbit will send data to HealthVault daily. Same thing is true with the MS Band. These types of bridges can help consumers become more motivated to use this EMR app.
I have a friend with multiple myeloma. I have helped her make her way through an unrelated network of 8 specialists. Only one of them has transitioned to EMR. My friend’s primary oncologist uses paper records and the stack of papers is at least 8″ high. This is pretty typical of oncology patients. The practice is totally intimidated by the prospect of going electronic.
Unfortunately, barriers to going electronic have not spawned the serious development of a field of EMR consultants (http://www.fortherecordmag.com/archives/ftr_01222007p34.shtml). Until that happens, I don’t think many practices will go electronic. And, until they go electronic, it is hard to imagine the widespread adoption of the patient-centered EMR.