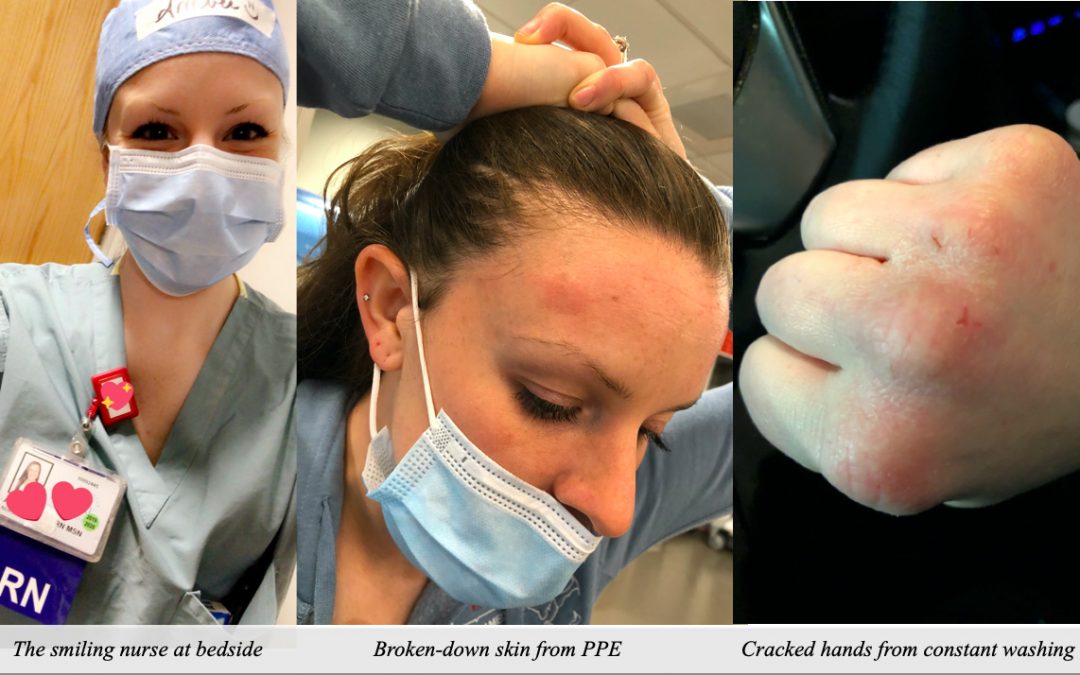
Editor’s note: This post is from Amber Soucy MSN, RN, a board member of our Society for Participatory Medicine. Like many front-line health workers she hides the stress (see her profile photo at right), but this era is tough in ways nobody ever signed up for, and this post covers an angle that’s all Amber: the difficulty of being kept away from the patient. (I myself created the photo composite in the header image, with her permission; it’s not something she submitted.) Here’s her post.
I’m a social person by nature. I love talking, interacting, and learning with and from others. Never in my career as a nurse did I think that I wouldn’t be able to be social.
COVID-19 has impacted all of our lives; some might be out of work and stuck at home, others might be struggling to make ends meet and are worrying about not being able to put food on their tables to feed their families. Me? Well, I’m a nurse so I’m on the front line. I work at a level 1 trauma academic hospital in Boston, MA and we are always booming. Patient after patient, code after code, we see and treat thousands of patients each week. Now with COVID-19, we have even more patients that are not only presenting to our facility but that are more critically ill.
One of my passions is improving the patient experience. I focus my efforts on strengthening the patient-provider partnership (I’m a board member of the Society for Participatory Medicine), and laying down a foundation of trust so that I can collaborate with my patients and allow them input in their plans of care. I spend time by the bedside, holding my patients’ hands, conversing about their past, present and future, and learning from them every step of the way. I care, I truly do.
But now, I can’t keep my line of communication open with my patients. Our communication is closed the minute I close their room doors. I don’t like knowing patients are closed off. I don’t want them thinking and feeling as if they are alone. I hate that we can’t allow visitors to cheer our patients up. I hate not being able to be present.
The mental and emotional toll that COVID-19 is imposing on healthcare professionals is unreal and truly unprecedented. I would hope that nurses and doctors entered the profession with the desire to help, care and treat. I mean, that’s definitely why I chose nursing as a career. But now this virus is wedging itself between my patients and me and it’s, by far, the biggest barrier I have ever faced.
The minute I leave a patient’s room and close their door, I leave them alone. They’re already riddled with fatigue and general malaise, but now I feel like I’m leaving them helpless and hopeless. And that’s exactly how I’m feeling too.
I cry almost every day and night thinking about how I wish I could have done more, how I wish I just could have been more present and caring. But I can’t, and it’s not by choice but rather because of the brutally crucial precautions to keep myself, my hospital community, and the community at large safe and healthy.
I’ve needed to accept that it’s okay to not be okay about this. It’s okay to feel, whichever end of the spectrum those feelings may land. We are all in this together and the more people know and understand this, the less alone we should feel. And the feeling of not being alone is the greatest and most important right now. We need it.







When I had my pancreatic surgery in August of 2019, Amber was my nurse and I can’t tell you how great she was while staying in the hospital, her encouragement, care and ways top make patient like me didn’t feel alone especially the kind of surgery. We talked almost everyday she’s in my room and I have never see an unhappy expression on her face, Amber does have th8 kind of magic power that makes everyone would like to be her friend and her professional aspect is undoubted. I am an Asian didn’t know how to express in a better way of Amber, so to make it short, Amber is a natural born nurse and angel. PERIOD!
I have had the absolute pleasure to work alongside Amber and I have no doubt the love and compassion she has for her patients and profession. She hits the nail on the head when she says how isolated this has made us feel. The separation it has caused between people is evident in all aspects of our lives, especially when trying to give care to our patients. We’re all going to need a massive group hug when this is over!!!
I am a patient being taken care of by Amber. I am not only a patient but I also work at the facility in a different department. While all the nurses her have been great for the past five days, Amber stands out more. Her energy and attention, love and care she has shown me is phenomenal. She tops it off with a great sense of humor and has taught me and reminded why I joined the medical field before she was born. I love caring for people and making them know they are not alone. Amber did just that. She is definitely one that can’t and should never be replaced.
My sincere respect Amber. I, too, was her patient last year. I think Amber is an example of what an ideal nurse should be. I know that now it is very difficult for medical personnel around the world. After all, a pandemic is really scary. Amber is always ready to help everyone. Thanks, Amber!
When I worked the floor I always kept the doors open. We could see each other , it gave the patients reassurance that there was always someone close by. Also , I liked to be able to look in when I walked past so that I could see if someone needed help. I can’t tell you how many times I was able to catch a problem before it happened/got worse . Closed doors would have driven me crazy ! So stressful, take good care of yourself! Hang in there!
Amber was really impressed with her professional skills, the ability to sympathize and choose the right words. I really hope that there is a person who will have the opportunity to reward this person in full. Or I propose to make some kind of surprise to her, whom she deserves!
As I read this and heard these heartfelt words, I thought of the many nurses on the front-lines battling COVID-19. They are here. They are making the time and they are doing so much good. Their contribution during this global pandemic is immense and their sacrifice extreme. Hospitals providing care for COVID-19 patients have quickly become a war zone. Thank you very much for sharing this. My prayers with these frontliner heroes.
It’s always great to read the stories of great personalities who live to serve like Amber. I respect and love what she did for the community and I’m using this moment to share my love for all those leading us from front to break this pandemic barrier.
Being a professional caregiver from a housekeeping company, I can relate myself to most of the situations we may run into and how we take care of it. The first and foremost thing in our thoughts are to give utmost care to the patients to help them have not only the physical well-being but also be peaceful mentally.
Kind Regards,
Jenny M
Caregiver at HousekeepingCo