Since November I’ve been blogging on my personal site about what happens when a patient tries to help control costs, in my cost cutting edition posts. Most recently I noted that this stuff takes time, especially since our glorious American healthcare system seems to be set up to block our access to what things actually cost … or at very best, we have no channels and pathways to let us find the information.
Well, ladies and gents, I’m fed up. I have to get on with life. I’ve been trying to be a responsible, engaged patient, and if the established channels won’t make it easy for me to find out what I need to protect myself, I will blow the whistle, announce what I’ve found so far, and move on. And we’ll take it from there.
I’m leaving today for 11 days of work in more sane countries – Switzerland and Holland – so I’m going to report the status here.
A caution and apology at the outset: I expect this will be read by some of the people I’ve spoken to at these companies. A lot of the frustrations I express here are because we couldn’t connect. I am grateful for your effort; you’re just too hard to reach, which is a problem if you’re the only one at your company who can help with this kind of work. I will appreciate your continued effort as we work through this change in American healthcare.:)
Later I’ll blog about the results of my research into my basal cell carcinoma. But for today, let’s just look at the simple (you would think) matter of getting an important CT scan.
The Simple Case: My Five Year Follow-up CT Scan
Five years ago right now, my cancerous kidney had been removed and we were preparing to begin interleukin on April 2. That means my upcoming semi-annual CT scan, here in 2012, is a biggie: the five year one. Among other things, lots of studies record the patient’s status five years out.
But I have a problem – a big one. On my $10,000 deductible insurance, my scan last fall cost me $1,736, and I’m not sure another one will be worth that to me.
Back then I blogged about how ridiculously non-transparent my “EOB” for that scan was – the “explanation of benefit” paper you get from the insurance company for each medical bill. I scanned it and posted it. Every single line item’s “description” of service was the single word “hospital,” and when I called the number on my insurance card for details, the agent actually said, “We have to trust whatever the hospital tells us.”
I later found out she’s wrong – misinformed, answering a question without being trained about it, or whatever. My point here is simply: look what happens when someone tries to help improve our out-of-control US health costs.
A key factor is that this is the only industry where you have to pay for something without line-item detail. I mean, can you imagine checking out of a hotel (or auto repair) and getting a bill for $1,736 with no line-item detail?? So that makes me ask, how did that happen, and how do we fix it? For my part, I’m going to ask and keep asking, and not take “nobody knows” for an answer.
So I decided to dig.
_________
As my next scan approached, I wrote to my oncologist, saying I wasn’t sure if I would do it. He said he’d prefer to have the data but he’d understand if I felt I couldn’t afford it. He pointed out that it’s the five year one.
I decided to find out what my options are. Could I get it done for less? Someone pointed out that my hospital offers discounts for people who can’t afford full price or don’t have coverage.
Hospital as shopping mall:
It turns out that to learn about this I had to call two different numbers, because most hospitals are like shopping malls: they’re big buildings with lots of common services, but most of the business that happens there is done by independent merchants. For one thing, this explains why the departments often are totally not connected to each other, any more than Abercrombie & Fitch is connected to Starbucks. (You might think two hospital departments share more mission for their customers than Starbucks and A&F do, but that’s not necessarily reflected in the business setups, much less the medical records)
So I had to talk to the hospital itself to learn about such discounts for the “facility charge,” and another group (in another city) to learn about discounts on the “professional fee” (physician charges). Long story short, each told me I’m not nearly poor enough. (I’m nowhere near poverty, which those discounts require.) I don’t mind being told that, but note that the people who told me to explore discounts didn’t note that requirement. So it took me four phone calls, with tag, to connect with someone who did know.
Side note: I half-expect to be told that this is wrong, and such discounts do exist for self-pay people like me. If so, it will bolster my point: the people I talked with didn’t have the right information. Disempowering.
Understanding my “shopping list”
To comparison shop, I need to know the shopping list. The insurance company literally didn’t know what was on the EOB, so they couldn’t tell me. They said I could only find out what the line items were by contacting my hospital.
The hospital’s patient portal supposedly lets you review your bill, but it’s all blobbed together into totals – no detail:
|
That’s fine for high-level detail, but there’s obviously no way to check it for errors (e.g. wrong insurance codes, services that didn’t actually happen), nor to explore what another provider would charge. So, the engaged / activated consumer has more work to do.
I called the hospital and asked where I could find detail. It’s not online – they have to print it and mail it to you. Then, to understand my actual cost, I had to take the printout and match up the prices with the matching list price on my “EOB,” to find my actual cost – the negotiated discount. (I had to match it manually because they weren’t in the same order, line by line.)
Side note: I will put “EOB” in quotes until the day when the damned thing actually explains anything.
As I said in that November post, I believe the FTC should prohibit calling something an explanation if nobody can understand what it says – not even the people in customer service!
It turns out the 15 line items break out into four categories: the scan itself, the radiologist who reads it, the bloodwork needed before the scan, and then the meeting with my oncology team to review it.
Comparison shopping
To comparison shop, I need to know, apples to apples, what I’m buying. (Buying? Yes, buying. Like a consumer.) I never did get anywhere near the level of detail I want, but in the process I learned enough to know what I’m going to do. Here’s how it went.
- Item 1: Lab work: armed with the specific test names, I called an independent lab, Quest Diagnostics. Turns out they’re more expensive than my hospital – yay for my hospital! (Hospital $248 through insurance, Quest $347)
- But wait – that’s Quest’s list price – what’s the price for each item if it’s passed through NHHP, my insurance company? Quest’s answer: “We don’t know.”
- I called NHHP, and they don’t know either.
Yes, folks, both the vendor and my insurance company say they don’t know.
That’s how I found out that the company I call (the number on my card) is not the actual one that negotiates prices with providers – the number I have just does the billing.
No wonder the person I first spoke to, last fall, had no clue about the line items. She (and the better-informed supervisor I eventually found) have no access to the information.
It turns out the business relationship with the doctors is actually through another company, American Healthcare Alliance. They negotiate the prices; the bill for a service goes to them. They apply their negotiated discount, remove the description of service, and pass it to the people who print my EOB.
So to find the negotiated price – remember, I’m trying to help reduce costs here – I have to call them. So I did. Sequence of events last Friday, March 23:
- The number I was given had this announcement: “Today is March 2. I’ll be out of the office until…. Please leave a message, or, for immediate assistance call Ms. X at xNNNN.”
- I left a cheery voicemail reminding her that her recording’s out of date, and called back to Ms X’s extension for immediate assistance.
- I left a message at 10 a.m. No call back yet.
Mind you, I can’t fault the company too much – they obviously don’t have great phone customer service practices, but I also know they’re not at all accustomed to people like me calling with questions like this. Still, this is what happens when a consumer tries to help control costs.
(Suggestion: let’s get them accustomed to fielding questions about costs.)
- Items 2 & 3: CT scan and radiologist: The bulk of the cost – $945 last fall – was for the scan itself. Then there was another $290 for the radiologist to interpret it, total $1235. Add the $248+ of lab fee = $1,484 so far.
- I know there are independent radiology shops – some advertise on TV – but I wasn’t looking forward to the research, because there’s nothing (yet) that remotely resembles the comparison sites we see for travel (Orbitz, Travelocity, or my favorite, Kayak.com).
- But then, through discussing this in social media and in conference hallways, I learned of the pricing standards site HealthCareBlueBook.com. (Analogous to the blue book for car prices.)
- On that site, you put in your zip code and select the service you want. For me it was
- x-ray → CT → Chest Without Contrast: expected price for my area $326, including the radiologist
- Plus, Abdomen/Pelvis Without Contrast: $411, including radiologist
- Total $737 – 40% less ($500) than the hospital. (This is the expected fee in my area, not a specific provider.)
This is still not great financially, but it’s substantial progress. (In my hospital’s zip code, downtown Boston, the amounts are $368 + $464 = $832 … so the book says I’d save $95 plus mileage & parking by using a local shop (free parking) instead of going downtown. Deal!) (Of course this assumes I can find one with good equipment and quality I trust.)
Then, salvation through the grapevine – I learned about Salem Radiology, in Salem NH, a half hour from here. Look:
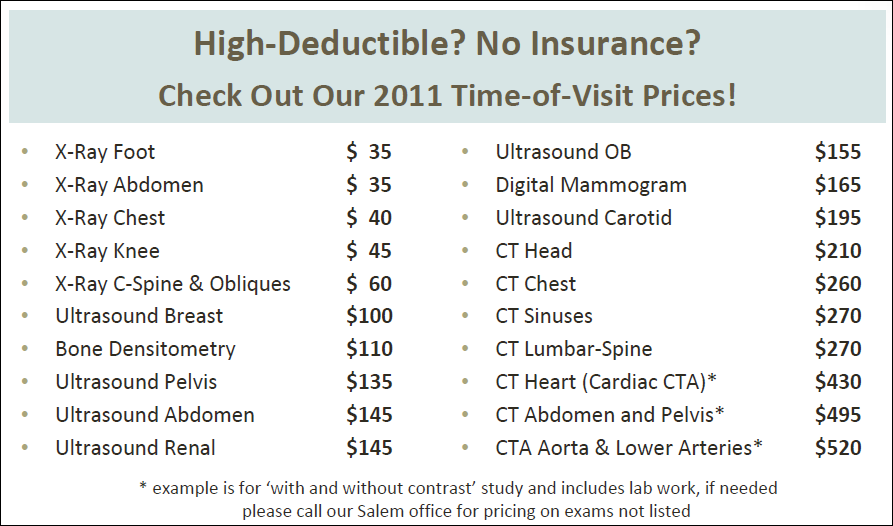
Look:
- CT of chest: $260
- CT of abdomen & pelvis is listed here as both with and without contrast; a phone call said that “just without” is another $260
- Total $520
- And the rest of that PDF and their site explain that all prices include lab work and the radiologist’s report
- Yes – the separate charges for lab work – $248 via insurance at my hospital or $347 from Quest? Included in the $520.
So, woah: now we’re down from $1,484 to $520.
It’s not a fly-by-night shop or cheapo; they’ve been in business since 1975, and seem to be continuously updating their equipment: “We’re proud to have been the first provider in the region to offer our community digital mammography (2004), 64-slice Cat Scan (2006) and 3T MRI (2009).” But they’re a retail business – no captive market, so they work to earn your business, with pricing designed for consumers like me.
Imagine that. Healthcare operating like a consumer business.
So, ladies & gents, it’s 99% likely that I will go ahead and get the scan that my oncologist recommends. (I also looked at other shops’ sites, but nobody else seems to post their prices. Salem is well below local “blue book” – $520 vs blue book $737 – so I’m doin’ it.)
- Item 4: Oncologist visit. Ironically – and distressingly – it leaves me with the matter of visiting the oncologist to discuss the results ($252 + drive time and parking), which for the past couple years has been mostly a (very happy) social visit. How odd would it be if I get the scan and just send the doctors the results, and ask if they really need to see me? (If they say I do, I will!)
In some ways this is upsetting to consider. But ladies and gentlemen, when costs are completely out of control and, increasingly, unaffordable, you can surely expect more consumers to do this. After all, many of us have been skipping care entirely – and then the industry writes articles about how we’re “non-compliant.” (I heard yesterday on New Hampshire Public Radio of a middle-class woman who hasn’t had a pap smear for years – has been uninsured, with kids, since her husband left.)
Will you fault us for trying to get care (being engaged, “compliant”), doing the hard work to find it at a price we can perhaps afford? Will you help?
For my part, I also have this skin cancer to remove (probably thousands), plus $3800 for unrelated dental work this month. And optical costs for my high intra-ocular pressure, which, if not tended to, could become glaucoma. All of those are more urgent – at the moment – than a five year follow-up scan.
==============
So here is the bottom line: the world is changing, now, and it’s going to hurt bad for some people, and create big opportunities for others.
- As costs keep rising, and more and more people decide “I’m not going to take it anymore,” more of us will start asking “What are my options?”
- Some will start to say “It’s my damned money,” and declare their own terms, issuing an RFP.
- As word gets out that prices vary this much, it’s going to get very unhappy for the people who can’t justify higher prices.
- Note: as in every industry, when this happens you can’t fault the people who’ve been high priced: they mostly didn’t set out to be that way. But it hurts when the change hits; I felt it when desktop publishing hit typesetting. Get ready for it.
- It will not be easy for big institutions with high overhead to adjust their pricing structure to be competitive. (In June 2009, business genius Clayton Christensen said the general hospital is not a sustainable business model. Yikes.)
- I’m very, very concerned for the wonderful people I’ve met who work in those institutions.
- Consumers who start shopping will create a great demandfor websites that aggregate different vendors’ prices – and, for radiology, the quality of their equipment and software.
- Travel sites tell you what type of airplane you’ll get, and their on-time performance. Watch for this in healthcare.
- It will also create a market – an ecosystem – for related services, such as cloud image services that are fully controlled by the consumer and easy to use. (The image reading software on my hospital’s scan CDs is free – as are the CDs – but the software’s extremely clunky.) Ecosystem examples in travel:
- SeatExpert and SeatGuru take your flight’s aircraft type and pull up a seating plan, to help you with seat selection. (Which seats don’t recline? Which have restricted legroom?)
- Tripit.com finds my confirmation emails and imports the schedule info (so my wife can view it on her Tripit app), then publishes it all in a Google Calendar that I can see on my phone.
- FlightStats.com connects to Tripit and looks up gate information for my flights, in real time, even if the gate changed while I was in the air.
- Addition, 9:30 p.m. – forgot it earlier!: This will be a very big opportunity for providers who switch to transparency. As in any other industry that gets truly disrupted – and I don’t mean upset, I mean disrupted, in Christensen’s formal definition – the dominant incumbents will deny that it’s happening, deny that it’s even possible. But a rapid increase in information liquidity – free flow of information, in the new ecosystem – will mean it’s much easier for new solutions to get noticed and to succeed.
The new world is starting to arrive, folks. I was about to walk away from a scan that, honestly, I would prefer to get but couldn’t afford. Now I probably will get it.
But I reached these results without a shred of help from the insurance industry … and with help from new-generation players.
We must take matters into our own hands, while demanding that industry – providers and insurance alike – give us a hand. Let Patients Help!
And innovators, have at it. Pounce. We need your help.
The Google Doc where I recorded my findings is at http://bit.ly/epdavescan





Hey Dave, what you are doing — isn’t that what Medicare automatically does, slash all fees to the bone (To the point that care providers are surely struggling to survive on the Medicare minimums).
Seems to me those of us who survived long enough to be on Medicare can count on Medicare to do our cost cutting. Tell me if I’m wrong…
Barbara,
I’m not so sure that this is slashing costs to the bone. I think it is picking the provider that is efficient enough to do the job well and at low cost.
When I was pregnant I needed a abdominal U/S (for the liver). The hospital where my doctor was practicing didn’t schedule it for 3 weeks, and then wouldn’t release the results for another week or two (waiting for a typist to write the report). In pregnancy this is a very long time. I found a local radiology shop that scheduled me in 2 days and released the report the day after the test.
I suspect they would have also given me a better price because they didn’t need to go through who knows how many third party providers to do the scheduling, typing, billing, etc.
In 2005 a doctor can’t type a report? Can you imagine having a secretary to type your emails or blog posts?
I know that hospitals have expenses like research, teaching, admin, etc. But I think they are using the excuse too much.
In terms of ecosystems, I’m curious if you see a role for direct primary care: http://www.dpcare.org/
Thanks so much for this post!
Dave,
I was thinking the other day how lucky we are to have you raise all these issues. I can only imagine how difficult it is to go through this and then documenting it for others.
I hope the people that can change these things will see how absurd the system is and do something about it. I don’t think we can ever thank you enough.
I wish the scan will turn out clean and you will get good prices for all other procedures!
Now THIS is what I call real healthcare reform: a patient acting like a customer, and seeking the best provider for a needed service.
Dave, you’ve been a leader in this arena for a long time now, and I’m hugely grateful for every single thing you do. I’ve been calling out the healthcare and health insurance industries myself for a long time, asking all the same questions you have. The more voices raised asking these very questions is what will drive healthcare toward a truly patient-centric model.
It’s time we all banded together, ripped away the curtain that hides healthcare/health insurance policy (revealing that the Great & Powerful Oz is really just a naked dude who’s managed to convince us he’s the Emperor), and demand that the system become both transparent and manageable by us. The patients.
Rock on, my brother.
Hey Dave. As you know, I used to be a lil’ billing guru before I got back into the hardcore clinical data game. I don’t know if I can give you any insight, but I can say this — the terminology you are looking for is ‘fee schedule’ (this one is for Medicare: https://www.cms.gov/apps/physician-fee-schedule/search/search-criteria.aspx . That one is normally what providers will use to determine their own pricing).
Part of the reason pricing is so secretive is because we don’t want people to know how we determine what the payment for services is going to be. And, cost is a notoriously difficult figure to wrap the mind around, especially in the hospital space.
Also, just FYI, the professional fee actually represents the ‘cognitive component’ of what a physician does (they are higher for more difficult tasks), so even if you don’t go in to see your oncologist, you’ll still get a bill for his interpretation of your scan, so don’t forget to figure that in as well. They would probably have to code it so that at the stand alone radiology shop, they would be able to charge both the technical (equipment part of the fee) and the professional — and you might get hit again with that pro fee at the doctor’s office.
Sorry. This is possibly more detail than you want. Or maybe not enough . ..
Not at all more detail than I want, Jamie – this isn’t a personal request for help, it’s a public exercise to see (and reveal and discuss) what happens when someone tries to control costs.
The comment stream becomes a sort of educational archive for others who come later, if the comments are useful. Yours is.
Another factor is that often the insurer and hospital have negotiated a capitated rate, where the insurer will pay X dollars per month per patient for all lab work of some type. This may make excellent business sense, but it makes the relationship between your bill, your tests, and the hospital actual costs very difficult to determine.
That’s the very “great and powerful Oz naked emperor behind the curtain” thing I was talking about in my previous comment. Health insurance should make it easier to pay for healthcare, but not at the cost of logic or access to cost structure. Procedure X should cost $Y for everyone who needs Procedure X. Since it doesn’t – we don’t have a single payer system, and I doubt that our nation’s cowboy/rugged-individualist mindset would allow for one – then we should be able to know going in exactly how much something will cost. Insurers don’t like it when we ask – takes their ability to run the game off the table – but we must keep asking. Never stop asking. Sooner or later they’ll realize it’s answer or … die.
I will send this to my business partner we were just talking about this recently!
I’m working on a curated compilation of tools for healthcare consumers who want to compare cost and quality – you’ve all taught me a lot already!
Here’s a resource I found just yesterday; it’s a contingency model business to seek lower procedure costs for individuals. I’m interested in hearing what others think.
MedicalCostAdvocate.com
And now, two years later, the prices have somewhat stayed the same. I’m relatively young and healthy, so insurance isn’t really my first priority but hopefully costs go down as I age.