 Care designers and fans of patient-centered care, listen up: a hat tip to Danish friend Malene Louise Djurhuus Laubinger for this, from The Guardian: How collaborating with patients improves hospital care.
Care designers and fans of patient-centered care, listen up: a hat tip to Danish friend Malene Louise Djurhuus Laubinger for this, from The Guardian: How collaborating with patients improves hospital care.
We’ve often said on this blog that participatory medicine can extend well beyond the care encounter, to the design of care itself. Ultimately, it leads to questions like “Who gets to say what care is?”, or this, from a talk I gave in 2012:
“If the microscope’s happy but the patient’s not,
has care been achieved?”
In short, there’s more to care than the biology and therapies. Those are important – but there’s more.
And, happily, this “more” is often cheap. This Guardian piece recounts several innovations that appear in no textbook, no med school course – they came from listening to patients about things that matter a lot to patients:
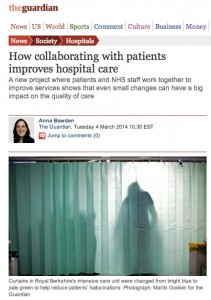
- A change in privacy curtain color reduced hallucinations in ICU patients
- Intubated patients were given an iPad app, to communicate, that had been developed for autistic patients
- Several other example that arose from listening to patients found valuable.
Some people in audiences I’ve spoken to have asserted that patients seem needy and self-centered. Well, consider this, about how it felt to these patients, to be collaborating to improve care:
One of the legacies of the project has been participants’ personal satisfaction. Lusby [the patient who identified the ICU curtain issue] says it was her chance “to give something back to the hospital because without them I wouldn’t be here”.
I know there are initiatives or anecdotes in the US and other countries like this, but I don’t know if they’re cataloged anywhere. Please share in the comments.





Recent Comments