Researching recently I wound up looking at where we were two years ago – February 2009, just as the Society for Participatory Medicine (SPM) was forming. Fascinating to see what topics were live then and are still relevant today – this community has focused on some great discussion, whose relevance has panned out well.
“Patients” vs. “Health Care Consumers”? Both, If You Ask AmyT
Healthcare’s going through social change, and in times like that, language can disturb people. This was our first post on what’s become an ongoing subject: do we call ourselves “patients” (a term that some find diminishing) or “consumers” (which some also find diminishing) or what?
This post covered the view of Amy Tenderich of DiabetesMine, who’s on the editorial board of our Journal of Participatory Medicine. Our most recent post on it is December’s A lot of shackling lives in language, which links to a good post by SPM member Fred Trotter.
Twitter, Facebook, and e-patients
From the Pew Internet Project’s first report on Twitter: “Twitter users engage with news and own technology at the same rates as other internet users, but the ways in which they use the technology—to communicate, gather and share information—reveals their affinity for mobile, untethered and social opportunities for interaction. …”
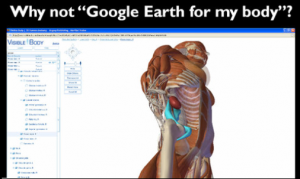 This post led to a line in a talk I gave in September, “Why not Google Earth for my body?” The idea was to “mash up” VisibleBody with my own digital CT scan data so I (or you) can visualize our actual innards. Then, voilà: in late 2010 Google announced the Google Body “body browser” —
This post led to a line in a talk I gave in September, “Why not Google Earth for my body?” The idea was to “mash up” VisibleBody with my own digital CT scan data so I (or you) can visualize our actual innards. Then, voilà: in late 2010 Google announced the Google Body “body browser” —
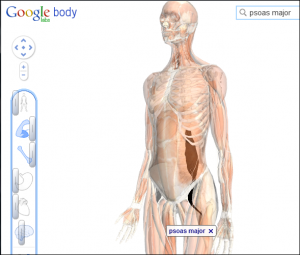 Visible Body is miles ahead of Google Body, but hey, we’re in this to create the future, right? I hope Visible Body will connect itself to many data sources, including digital scan data.
Visible Body is miles ahead of Google Body, but hey, we’re in this to create the future, right? I hope Visible Body will connect itself to many data sources, including digital scan data.
Why? Because I’ve heard repeatedly that people change behavior better when they’re looking at their own situation, vs generic advice. And in healthcare, outcomes don’t change if behavior doesn’t change.
A business-oriented discussion of why any attempt to change the business of healthcare was going to meet terrific resistance, because if you cut costs 10% in a trillion dollar industry ($100 billion), it means somebody is going to lose $100 billion of income. And that won’t happen easily. It became apparent that we consumer/patients must be responsible for our own improvements.
Medpedia: Who gets to say what info is reliable?
Discussion (with 68 comments) of the newly announced “medical wikipedia,” based on the skewy view that any info vetted by health professionals is trustworthy, and anything that’s not is not. In particular see our John Grohol’s excellent discussion in a Feb 24 comment on how wrong their article on depression was – despite being vetted by a certified professional.
It’s important for e-patients and providers to understand this: the info professionals have can be seriously out of date, and people need to be open to other sources.
Why Technology is No Longer Optional in Public Health
A short link to a post by @MindofAndre on mobile tech’s potential. He was right: two years later mobile health / mHealth is hot, with annual conferences and a whole Pew Internet report; our most recent post is “it’s not just phones and browsers,” and see Susannah Fox’s talk at Mayo Transform conference. If you want to anticipate the future, keep tabs on Andre.
Participatory medicine might have reduced this tragedy
A terrible story where blind trust led to disaster at a famous medical center; being an engaged patient and family may have made all the difference. “For me this story triple-underscores the importance of every patient, caregiver and provider embracing the principles of participatory medicine. Medicine is too complex today for any one group to bear all the responsibility – even great doctors. And we as patients need to understand that our lives are on the line, AND we can make a difference.”
MedPage: Negative Data on Seroquel Suppressed by Drug’s Maker
Our first post on what’s been a distressingly steady subject: corruption in marketing of medications. To this day I don’t understand why people in an industry that makes miraculous medications (which saved my life) sometimes feel compelled to lie, knowingly or callously unknowingly causing people harm. It’s simply essential that informed, engaged patients know about this when they participate in decisions about their treatments.
In this case the drug maker reported to the FDA that they’d run several trials with the drug, and knowingly hid the fact that most of the trials didn’t work out well, and in fact caused harm.
——
February 2009 was also when Congress passed the Federal stimulus bill (ARRA), including the HITECH provision to encourage healthcare to modernize through the “meaningful use” of health IT. By February 2010 intense discussions were underway in Washington to define that. Members of the Society for Participatory Medicine submitted testimony at several meetings. A few highlights from that month:
- Participatory Medicine in Time magazine: Cancer community ACOR was highlighted, along with numerous other e-patients and resources.
- Meaningful use testimony – requests for your input What to do about “the cream of the crap”? ONC’s Adoption/Certification Workgroup meeting and results Testimony submitted to the Adoption/Certification Workgroup for its Feb 25 meeting
- Health IT executive Denny Porter also proposed that we create bridges between all the various Federal health records systems: Proposal for a health data system to support urgent cancer patients and wounded warriors
Finally, every February 28 is Rare Disease Day – “Alone we are rare. Together we are strong.” Rare Disease Day 2/28/10:
“One profound shift in healthcare enabled by the internet is the Web’s ability to be a common platform for huge numbers of low-volume diseases. This is the “long tail” effect that makes Amazon and eBay a success, selling vast numbers of items you never would have seen before the Web.
The difference, of course, it that this isn’t about obscure books; in this case lives are at stake.”
We hope to keep using this blog to host discussions about the present and the future that will help advance the cause of participatory medicine. Thanks for reading and thanks for your many great comments.
——-
Are you a member of the Society for Participatory Medicine? Our two content-related projects – this blog, and the Journal of Participatory Medicine – are free and open-access. For funding we rely on philanthropy and unrestricted corporate memberships (see our membership page), and almost all our work is done by volunteers (volunteer here) and individual members (just $30 a year). Participate – help create the future of participatory medicine!






Thanks for the retrospective, Dave! I was doing the same thing today — reading a current story, thinking of a year-old post:
Today’s Washington Post:
Is Google getting worse? The search giant’s results are suffering because of spammers
http://wapo.st/fdCKAK
One year ago on e-patients.net:
Health Sites: Some Are More Equal Than Others
http://j.mp/4xTLZZ
Did you see the tweet that went around about a month ago? Along the lines of “I read something in the mainstream news, but I couldn’t confirm it on a reputable blog.”
Wow, Susannah, that’s a terrific WaPo wrap-up of the situation with spammy sites and “content farms” messing up Google’s effectiveness. I used to work in search engine marketing, and apparently I faded out just as that business was cranking up.
I sure agree about the feebleness of eHow’s answers for a lot of things, though for trivial things they’re a shortcut to quick answers.
Google’s “onebox” search results for health are a separate problem, si? In that case Google has business arrangements with content providers, whose content is not necessarily optimal.
I’ll say more about that in another comment.
Susannah’s link to her 1/21/2010 post about Google’s “onebox” search results led me to check how that’s going. Last year she got 119 comments (!) – quite a debate about both the commercial relationship with those highly-placed content providers and the not-necessarily-optimal quality of that content. It certainly is not curated by anyone who knows the subject – it’s just plain old paid-for space, and they slap up whatever the provider gives them, right or wrong.
I tested it by googling kidney cancer (my disease) and checking the information displayed about Interleukin-2, the treatment I got. History of information:
Here’s what’s shown about interleukin-2 in the four sources in Google’s “onebox.” Note: my ACOR community pointed out first and foremost that IL-2 is the only thing that sometimes approximates a cure. See if that appears in Google’s curated info:
Bottom line: From my perspective as a patient, the info Google provides is pretty much garbage; based on this, I wouldn’t count on it for anything more than a first orientation to a subject.
And that brings me back to the point the Washington Post article made: the woman with the TV problem found Google’s results useless … but her social network got answers she could use.
We live in interesting times. Thanks, Susannah.
Thanks for the retrospective! This was quite a stroll down memory lane… Keep up the great work :-)
Me parece loable y maravilloso lo que estan haciendo, gracia a Dios estoy sana pero si me gustaría ayudar o apoyar de alguna manera, mi madre que ya esta descansando tuvo varias enfermedades de las mas fuertes y raras con ella experimentaban prácticamente y se como se sufre, sigan adelante.